Fibroids
Fibroids are common non cancerous growths that are found predominantly in the womb. They are made of muscle and fibrous tissue and vary in size. They can also be called myomas or leiomyomas and often appear during the childbearing years

Symptoms
Whilst many women have no symptoms, fibroids can cause heavy periods with flooding and clots that can be very distressing. Bleeding can also happen between periods. Pain is not usually a feature of fibroids but in some cases where the fibroids are large pain/discomfort can be felt in the pelvis or back as well as with intercourse. They can also cause increased menstrual cramps and period pain.
Large fibroids that are near the bladder can cause an increase in the desire to pass urine (urinary frequency). The length of periods can last longer and there may be a general feeling of fullness in the abdomen.
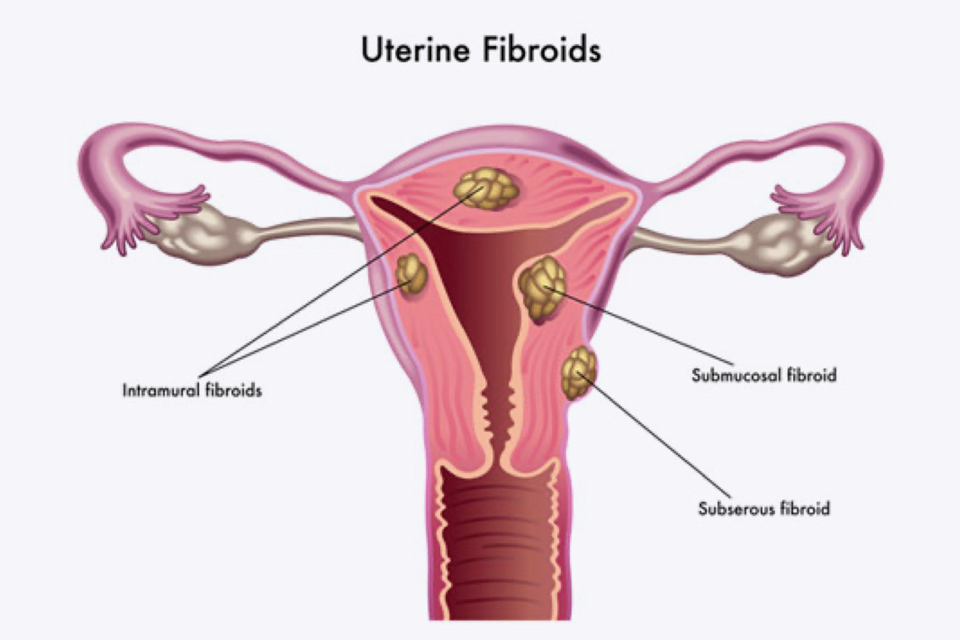
Types
There are four main types of fibroids.
- Intramural fibroids are the most common type of fibroid. They develop within the muscular walls of the uterus, as they grow they stretch the womb causing it to become enlarged.
- Subserosal fibroids form on the outside of the uterus and can become quite large in size before causing any symptoms.
- Pedunculated fibroids grow from a stalk on the outside of the uterus and rarely cause symptoms.
- Submucosal fibroids form within the wall of the uterus but push inwards into the uterine cavity, these usually cause the most symptoms and even small submucosal fibroids can be problematic.
Who is affected?
If you have a female relative with fibroids, then there is a greater chance that you will also suffer from fibroids.
Hormones play a role as fibroids are oestrogen sensitive. Increased levels of oestrogen, during pregnancy or by taking the contraceptive pill for example, can cause an increase in size or risk of developing fibroids. Conversely after the menopause fibroids usually shrink due to the low amounts of oestrogen in the body.
Lifestyles also play a role in fibroid development. For example, eating red meat, drinking alcohol and drinking caffeine have been shown to increase the risk of developing fibroids. Being overweight or obese also puts women at an increased risk of developing and growing fibroids.
When to see a doctor?
If you have the following symptoms, then it is time to see a specialist such as Mr Broome:
- If you have lower abdominal pain that doesn't seem to go away despite you trying to alleviate your symptoms.
- If your periods are long, heavy and painful
- If you have bleeding and spotting between your periods
- If you feel tired and appear to be suffering from anaemia due to prolonged bleeding
- If you have problems of frequency passing urine
Diagnosis
Diagnosis tends to be by ultrasound or an MRI scan (magnetic resonance imaging scan) which can look at the size, number and the position of fibroids.
Alternatively Mr Broome might suggest that you have a hysteroscopy. This is a small camera which is inserted into the vagina, through the cervix and up into into the womb to check for abnormalities.
It also may be necessary to have a laparoscopy (keyhole surgery) where Mr Broome makes a small incision in the belly button to insert a camera into the abdomen to examine the womb for fibroids or other problems.
What treatments are available?
Treatment is only generally required if fibroids are affecting your quality of life. If your periods are not heavy and you have no other symptoms then it may be better to continue without treatment, medication or surgery.
Medicines
Hormonal medication is one treatment option. These medicines, such as birth control pills contain progesterone and can reduce the amount of flow and the pain associated with heavy bleeding. Contraceptive injections or implants can even stop periods altogether.
Non hormonal medication may also be prescribed such as tranexamic acid or non steroidal anti-inflammatory drugs such as mefenemic acid or ibuprofen.
Surgery
There are a variety of surgical options available to Mr Broome to assist you. The decision as to which procedure is best placed to help you will come after a consultation and investigations.
Endometrial resection may be an option for you, it is a minimally invasive procedure (a camera inserted into the womb via the vagina) which can remove symptomatic submucosal fibroids by shaving them away.
Myomectomy may be the only option to remove fibroids if they are very big, the surgical procedure is performed under a general anaesthetic usually through a bikini line incision where the fibroids are then removed. There is a small risk of hysterectomy with this procedure so careful consideration must be given to the risk v benefits.
Uterine artery embolisation is a day case procedure undertaken in the x-ray department where the blood supply to the fibroid is blocked using a fine catheter introduced into a blood vessel in the groin, this causes significant shrinkage of large fibroids.
Finally, a hysterectomy may be decided as the best course of action if you have large fibroids not amenable to conservative treatment. For clarification, a hysterectomy is the surgical removal of your womb (uterus), ovaries can often be left in place which will avoid menopausal symptoms. There are different types of hysterectomy (vaginal, abdominal or laparoscopic) and Mr Broome can discuss these options.

